You are here
Urgent Action Needed to Shore Up Medicare Program
2014 Social Security & Medicare Trustees Reports
HIGHLIGHTS
This week, the Medicare Trustees released a report that warns of a serious shortfall in funding for the Medicare program, which provides health insurance to people who are ages 65 and over or disabled. Without reforms, the Trustees estimate1 that:
- The beneficiary population will grow by one-third over the next ten years as the baby boom generation turns 65 and becomes eligible for benefits. Within 10 years, over 70 million people will be enrolled in the Medicare program, compared to 54 million today.
- Medicare spending, which equals 3.4 percent of GDP, will grow by 22 percent over the next 10 years. Over the next 25 years, it will grow by 62 percent or more.
- The Hospital Insurance (HI) Trust Fund will be depleted in 2030—16 years from now. At that point, Medicare will be unable to cover 15 percent of its hospital claims.
MEDICARE IS A LARGE SHARE OF THE BUDGET, AND IT IS PROJECTED TO GROW
Medicare spending is projected to rise significantly in coming years. Per capita healthcare costs have been growing steadily for more than four decades, though their growth has slowed recently. This growth slowdown is unquestionably good news, but the causes and sustainability of it are unclear — some of the reduced growth may be due to the weak economy, and some may be due to increased efficiency. Importantly, the Trustees have incorporated this data on the recent slowdown in growth of healthcare costs into its projections. Even with these more modest growth projections, the Trustees project that Medicare spending will continue to climb as a percent of gross domestic product (GDP)—rising from 3.4 percent of GDP in 2014 to 5.6 percent of GDP within 25 years — an increase of 62 percent over that period.
Medicare spending is projected to rise by 62 percent within 25 years
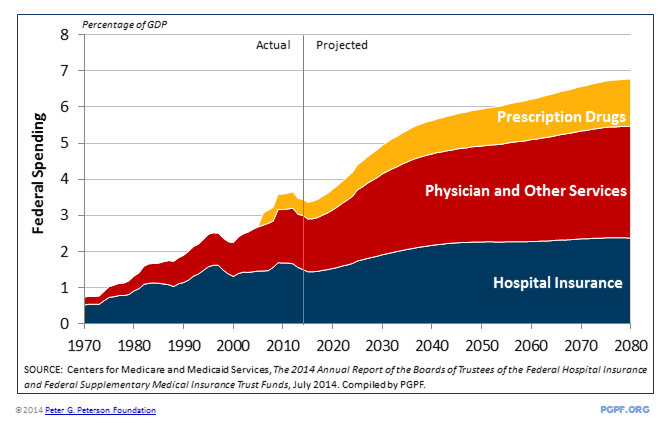
Medicare will also take up a larger share of the federal budget. In 1970, Medicare expenditures accounted for just 3 percent of total spending. Now, Medicare accounts for 15 percent of the federal budget, and is projected to grow to 18 percent of the budget by 2040.
Medicare is a growing share of the federal budget
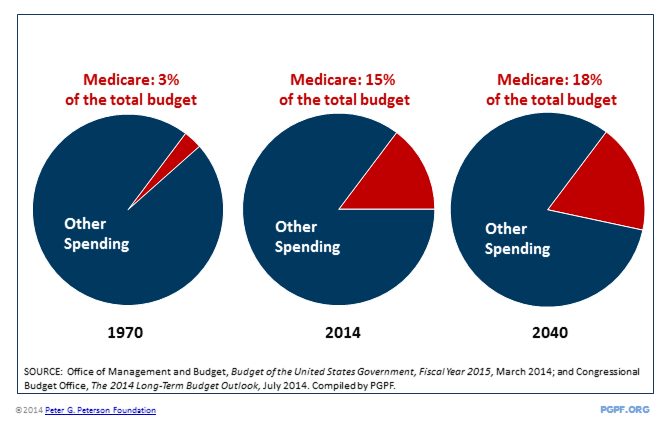
WHAT IS DRIVING MEDICARE'S HIGHER PROJECTED COSTS?
Projected Medicare spending growth is driven primarily by two factors: the aging of the population and rising healthcare costs per person.
The aging of the population is a major factor driving Medicare spending over the next 25 years. As the baby boom generation turns 65 (a milestone that began in 2011), they become eligible to enroll in the program. In addition, Americans have been living longer. In 1970, the average 65-year-old male was expected to live until age 79; today, he is expected to live until 84; within 25 years, he is expected to live until 86. The comparable life expectancies for women are 84 in 1970, 86 today and 87 in 2039. This is a welcome trend that is expected to continue, but it means Medicare recipients will receive benefits for more years than they have in the past.
The baby boom generation will boost Medicare enrollment
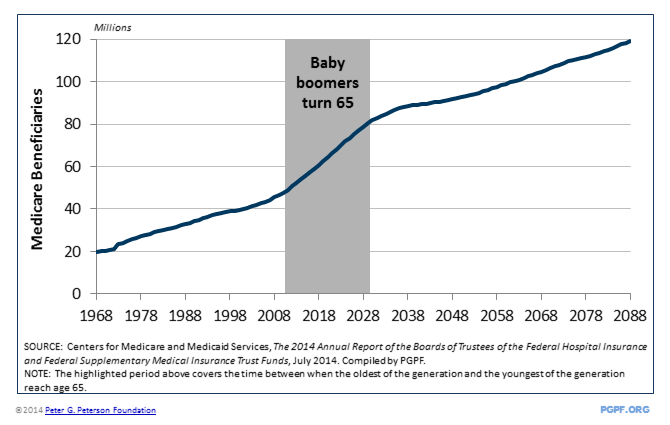
In addition to these demographic factors, the cost of healthcare for each Medicare beneficiary is also growing. The average cost per Medicare beneficiary (after adjusting for overall inflation) has tripled over the last thirty years. The annual cost is now about $12,000 per beneficiary. Despite the recent slowdown, healthcare costs are expected to continue growing in the years ahead.
The average per beneficiary cost of Medicare has tripled over the last 30 years, adjusted for inflation
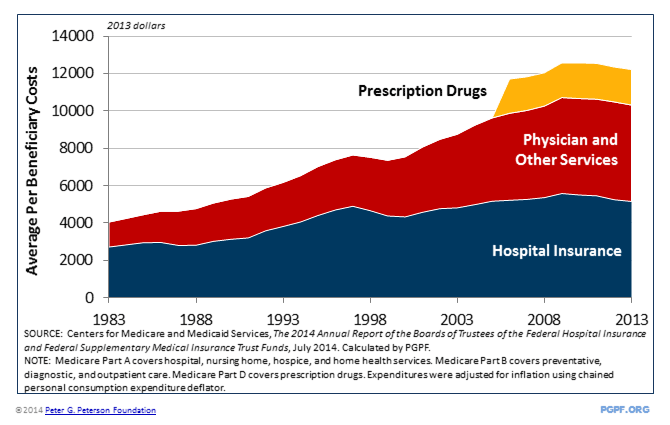
MEDICARE FINANCING PUTS PRESSURE ON THE FEDERAL BUDGET
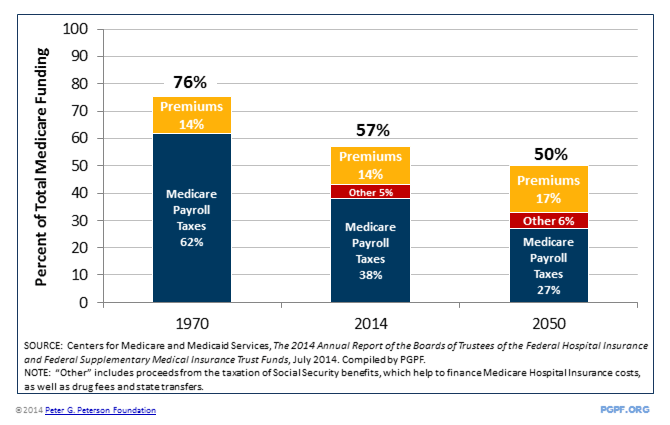
As a result of these and other factors, payroll taxes and premiums have been covering a shrinking share of Medicare costs. In 1970, Medicare was largely self-financing: 75 percent of its funding came from payroll taxes and premiums; the rest came from transfers from the general fund. Within 25 years, only half of the Medicare program will be self-financed; the rest will be funded by general fund transfers — putting more pressure on the rest of the federal budget.
The Medicare program faces a declining ability to fund its own costs, increasing pressure on the overall federal budget
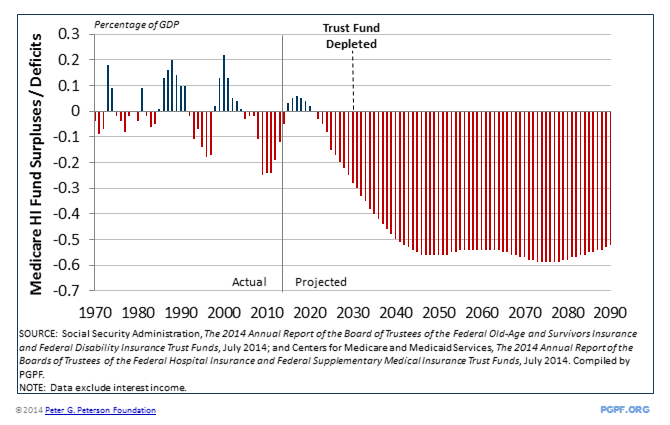
The Trustees project the Hospital Insurance (HI) Trust Fund will be exhausted in 2030. The HI program finances in-patient hospital care, skilled nursing, home health, and hospice care. Almost all Americans ages 65 and older are eligible for HI, which is largely supported by HI payroll taxes. Unless policymakers act, the Trustees estimate that in 2030 Medicare will be unable to pay 15 percent of its HI bills.
The cash flow of Medicare’s Hospital Insurance program will turn permanently negative in 2022 and the HI Trust Fund will run out by 2030
Medicare’s budgetary challenges go beyond hospital insurance. The Trustees also project rising spending on physicians, prescription drugs, and other healthcare services, which are programs funded by beneficiary premiums and general revenues. The trust fund for these programs cannot technically run out of money under current law because premiums and general revenue contributions are set annually to fully cover costs. However, rising costs increase the financing burden, placing pressure on the federal budget and constraining funds available for other programs.
MEDICARE COSTS ARE PROJECTED TO RISE EVEN HIGHER UNDER MORE REALISTIC POLICY ASSUMPTIONS
The Trustees issued three projections reflecting different policy assumptions: a current-law projection, a baseline projection, and an alternative projection. The current-law projection is optimistic for two reasons: it assumes that physician reimbursements will be cut by 21 percent in April 2015 (as required by current law), despite the fact that Congress has waived those cuts every year since 2003. It also assumes that certain cost-control provisions of the Affordable Care Act (ACA) will remain in place and be effective.
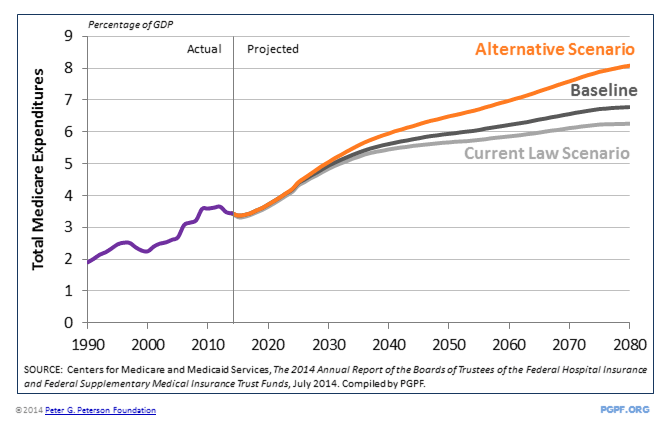
The Trustees’ baseline projection is less optimistic than the current-law projection because it assumes that physician reimbursements will not be cut. However, it does assume that the cost-control provisions in the ACA will be as effective as under the current-law projection. Lastly, the Trustees prepared an alternative scenario that assumes both that the scheduled cut to physician reimbursements will not occur and that cost-control provisions of the ACA will be ineffective or will not be implemented. In that scenario, the Trustees project that spending could rise to 6 percent of GDP in 2040 — 73 percent above today’s levels and 9 percent higher than the level projected under the current-law projections.
Despite the recent slowdown in Medicare cost growth, spending on the program is projected to rise sharply in coming decades
CONCLUSION
Medicare is facing a long period of growing spending due to the retirement of the baby boomers and increases in longevity, as well as rapid growth in healthcare costs. The Trustees call on Congress and the administration to act "with a sense of urgency" to address the growth in expenditures and the exhaustion of the HI Trust Fund. If done promptly, policy changes can be phased in gradually, minimizing the impact on current beneficiaries. However, if Congress and the administration continue to delay needed reforms, Medicare enrollees could see more significant and sudden changes to the benefits that they rely on.
For more information about trust funds, please see the following Budget Explainer:
1Except where noted, all projections in this document reflect the Trustees’ intermediate set of economic and programmatic assumptions. (Back to citation)
