You are here
Medicare Trustees Project Serious Financial Shortfalls
This week, the Medicare trustees released a report that warns of a serious funding shortfall in the Medicare program, which provides health insurance to 55 million people who are ages 65 and older or disabled. The program covers a wide range of healthcare services, including hospitals, skilled nursing facilities, home health, physicians, and prescription drugs.
According to the report, an aging population and rising per-enrollee healthcare costs will drive sharp increases in Medicare spending, which will not keep pace with the program’s funding sources. The trustees are calling on policymakers to act with urgency to shore up this essential program.
Absent reforms, the trustees project that:
- The beneficiary population will grow by one-third over the next ten years as more of the baby boom generation turns 65 and becomes eligible for benefits. In just 10 years, 75 million people will be enrolled in the Medicare program, compared to 57 million today.
- Medicare spending will climb from 3.6 percent of GDP today to 5.6 percent of GDP in 2040 — an increase of nearly 60 percent.
- The Hospital Insurance (HI) Trust Fund, which finances in-patient hospital and other expenses, will be fully depleted in 2028 — two years earlier than projected last year, and just 12 years from now.
The trustees urge lawmakers to enact legislation soon to put Medicare on a sustainable path:
"Notwithstanding recent favorable developments, current-law projections indicate that Medicare still faces a substantial financial shortfall that will need to be addressed with further legislation. Such legislation should be enacted sooner rather than later to minimize the impact on beneficiaries, providers, and taxpayers."
Medicare Spending is Projected to Climb Sharply
According to the trustees, Medicare spending remains on a significant upward trajectory. The trustees project that Medicare spending will climb significantly as a percent of gross domestic product (GDP) in the decades ahead — rising from 3.6 percent of GDP in 2016 to 5.6 percent of GDP in 2040. This is an increase of nearly 60 percent.
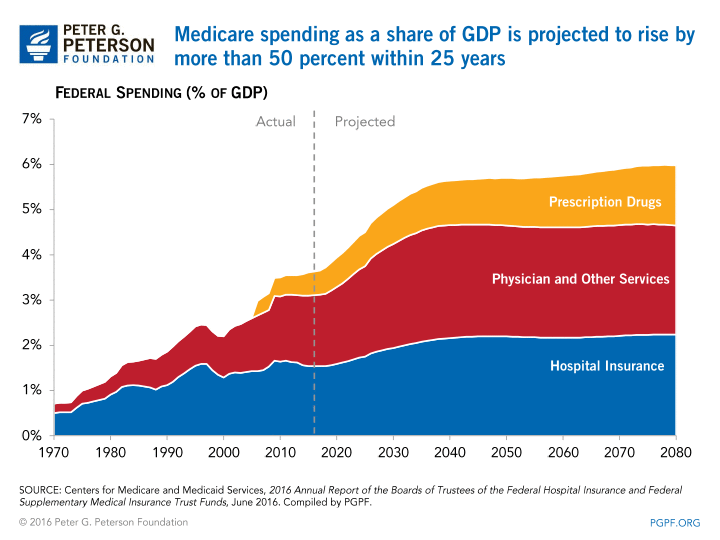
As a result of these increases, Medicare will also take up a larger and larger share of the federal budget. In 1970, Medicare expenditures accounted for just 3 percent of total federal spending. Today, Medicare accounts for 15 percent of the budget, and by 2040, it is projected to grow to 20 percent of the budget.

What is Driving Medicare’s Growing Costs?
Projected Medicare spending growth is driven primarily by two factors: growing numbers of beneficiaries due to demographics, and rising healthcare costs per beneficiary.
The aging of the population is a major factor driving Medicare spending over the next 25 years: as the baby boom generation of 76 million people turns 65, enrollment in Medicare will balloon. In 1990, there were 31 million people ages 65 and older; today, there are 49 million; within 25 years, there will be 83 million.

In addition, Americans have been living longer, which increases the length of time that beneficiaries are served by the program. In 1970, the average 65-year-old male was expected to live until age 79; today, he is expected to live until 84; within 25 years, he is expected to live until 86. The comparable life expectancies for women are 84 in 1970, 87 today, and 88 in 2040. This trend is welcome, but it means Medicare recipients will receive benefits for more years than they have in the past. In addition, medical costs are typically greater for those individuals who reach higher ages, further driving increases in costs.
In addition to these demographic factors, the average cost of healthcare for Medicare beneficiaries is growing, and has been growing for more than four decades. In fact, the average cost per Medicare beneficiary (after adjusting for overall inflation) has more than tripled over the last forty years: the annual cost is now approximately $13,000 per beneficiary.
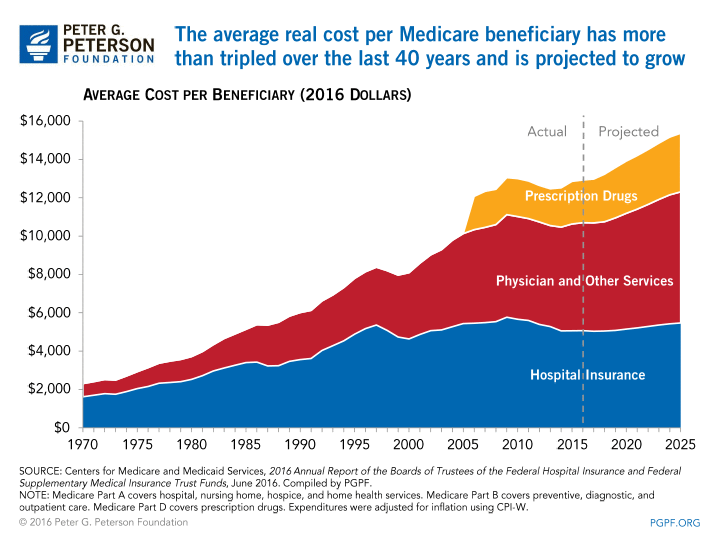
Although the rate of cost growth per beneficiary has slowed recently, some portion of the slower growth is due to the weak economy and will likely be temporary. In any case, because of the large projected increases in the number of beneficiaries, total spending on Medicare will climb sharply in coming years.
Medicare Financing Puts Pressure on the Federal Budget
As Medicare spending has risen, the revenue sources that are dedicated to fund the expenditures — payroll taxes and premiums — are covering a smaller and smaller share of the actual costs. In 1970, Medicare’s dedicated income (payroll taxes, premiums, and other) was able to fund 75 percent of the program, with the balance coming from transfers from the general fund of the Federal government. Today, dedicated income is only able to fund 52 percent. These shortfalls put increasing pressure on the rest of the federal budget.
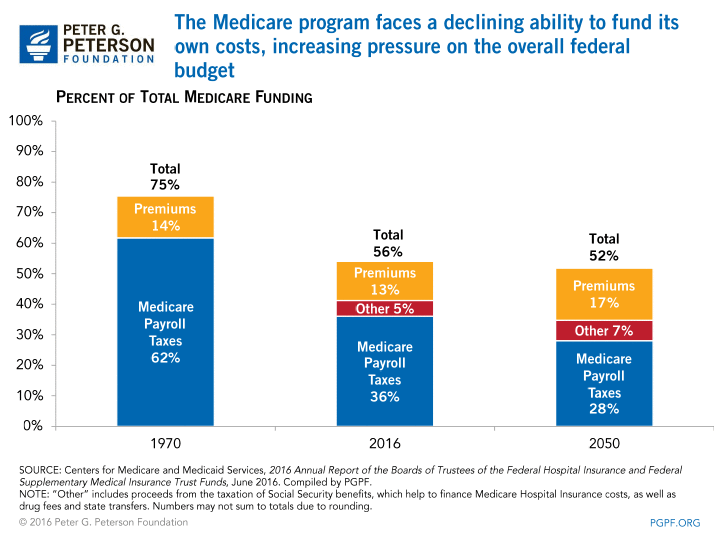
As a result of the imbalance between revenues and costs in the Medicare program, the trustees estimate that Hospital Insurance (HI) Trust Fund will be fully exhausted by 2028. The HI program finances inpatient hospital care, skilled nursing, home health, and hospice care, and almost all Americans ages 65 and older are eligible. Once the HI Trust Fund balance reaches zero, spending on benefits cannot exceed incoming revenues and premiums — unless policymakers act, the trustees estimate that in 2028 the Medicare program will be unable to pay 13 percent of its HI bills.

Medicare’s budgetary challenges go beyond hospital insurance. The trustees also project rising spending on physicians, prescription drugs, and other healthcare services, which are programs funded by beneficiary premiums and general revenues. The trust fund for these programs cannot technically run out of money under current law because general revenue contributions must automatically cover any shortfalls in annual funding. However, the rising costs for these other health expenditures put pressure on the rest of the federal budget, constrain funds that could be used for other programs, and ultimately lead to higher levels of federal debt and interest costs, which hurts the economy.
Medicare Costs Will Be Even Higher Under A Less Optimistic Scenario
The trustees provide two projections reflecting different policy assumptions: a current-law projection and an alternative projection. The current-law projection assumes that certain cost-control provisions of the Affordable Care Act (ACA) and the Medicare Access and CHIP Reauthorization Act (MACRA) will remain in place and be effective. The trustees prepared an alternative scenario which assumes that these cost-cutting measures will be ineffective or will not be implemented. In that scenario, the trustees project that spending could rise to 6.2 percent of GDP in 2040 — 72 percent above today’s levels and 10 percent higher than the level projected under the current-law projections.

Conclusion
Medicare is facing a long period of rapidly growing spending due to the retirement of the baby boomers and increases in longevity, as well as continued growth in healthcare costs per beneficiary. The trustees call on Congress and the administration to act "with a sense of urgency" to address the growth in expenditures and the coming exhaustion of the HI Trust Fund. If done promptly, policy changes can be phased in gradually, minimizing the impact on beneficiaries. However, if Congress and the administration continue to delay needed reforms, Medicare enrollees could see more significant and sudden changes to the benefits that they rely on. Policymakers should work together to stabilize and strengthen this important program for generations to come, while also relieving the pressure it places on the rest of the budget.
